Nurturing Smiles: Insights from Barbara Delage's India Visit
An interview with Smile Train’s Director of Global Nutritional Programs

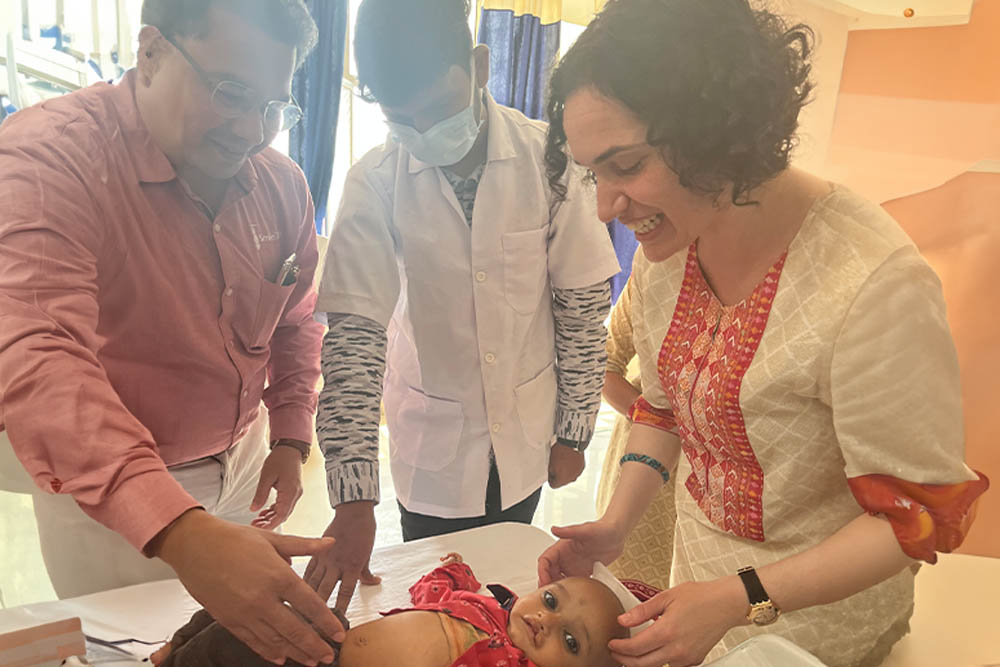
Children with clefts are uniquely vulnerable to malnutrition and related growth problems, putting them at increased risk for infection and morbidity. And life-transforming cleft surgery cannot happen on a child who is dangerously underweight. As Smile Train’s Director of Global Nutritional Programs, Dr Barbara Delage works each day to strengthen our partners’ lifesaving cleft feeding and nutrition programs, helping ensure our patients grow healthy and strong — and are ready for cleft surgery at the soonest safe time. She visited India recently to check in on our patients and programs here, and graciously took some time to talk to us about these vital initiatives and state of cleft nutrition in India.
How long have you been working for Smile Train? Have birth differences, including clefts, always been your speciality?
I am a biologist with specialist training in nutrition and food science and public health nutrition. I started to learn more about orofacial clefts in 2018 when I was involved in examining the nutritional situation of children with clefts treated by Smile Train’s partners worldwide. Following this first collaboration with Smile Train, I investigated the limitations and opportunities of Smile Train’s nutrition programs in Africa in 2019 and led an intervention in Western Kenya to promote the systematic examination of all babies’ palates at birth in 2021.
Is there anything that you would like to share with us from your interactions with partners in India that stood out for you?
I met with healthcare professionals eager to do well and find solutions to overcome the challenges they face in trying to respond to the needs of patients and their parents. A prominent aspect of nutrition care provision to any child, including children with clefts, is growth monitoring and promotional activities. Yet, Smile Train partners often have difficulties following up with patients after the initial consultation, especially those who live far away from the nearest cleft treatment centre.
During my visit, partners shared with me some of the solutions they identified to encourage more families to follow-up, including through remote patient monitoring and telehealth consultations and through actively collaborating with Accredited Social Health Activist (ASHA) workers. Adopting such solutions is essential to reducing malnutrition and other poor outcomes in our patients.
What is the most important aspect of nutritional support that needs to be addressed for children with clefts?
Nutrition support is not about giving food to patients – it is about creating the conditions that ensure children with clefts grow and thrive. Growth monitoring, feeding counselling, and nutrition care provision are all part of the continuum of feeding and nutrition care that Smile Train aims to strengthen at every partner hospital.

The lack of awareness of clefts and of the feeding difficulties of infants who have them is a major challenge to ensuring these children’s healthiest start in life. If entrusted with the skills and responsibility to create a positive impact, hospital staff providing maternal and child healthcare are in a unique position to address eating, drinking, and swallowing difficulties in cleft-affected babies and children.
While visiting partners in India, I discussed the key role of growth monitoring and promotion to support individual child growth and development and the need to prioritize the collection, interpretation, and utilization of accurate measurements (mainly weight and height) to inform decision-making regarding the care they provide to children with clefts.

Can you cite a barrier to preventing malnutrition in children with clefts in India and how could it be addressed?
There are multiple and very diverse factors that contribute to the increased prevalence of malnutrition in children with clefts. While timely provision of skilled feeding assistance can help promote good nutrition and healthy growth, some parents may delay bringing their child to a treatment centre.

In Varanasi, a couple came to the partner hospital with their three-month-old baby for the first time. When asked why they did not bring the baby shortly after birth, they said they decided to wait until their baby reached the minimum age for cleft lip surgery. This shows that there is a need to promote cleft care provision differently, focusing less on the age suitable for treatments and more on patients’ growth, development, and well-being. Care should start as early as possible after birth and be provided by skilled feeding and nutrition specialists to ensure that children are growing well and are healthy enough to undergo treatments.
What is your message for parents of children with clefts and the nutrition experts who work with them?
To parents in India and elsewhere, I say that Smile Train and our partners are dedicated to providing all the care that your child needs when they need it. I know it can feel overwhelming to be the parent of a newborn with a cleft and that feeding may be more complicated than what you were expecting. Yet, feeding and nutrition are critical and central to your child’s development, well-being, overall health, and future and should be your number-one priority. You must also understand that appropriate feeding and nutrition are key to the success of surgery and other treatments. There are solutions to overcoming feeding difficulties and Smile Train is working hard to make support from lactation consultants and other feeding and nutrition specialists available at all of our partner hospitals.

To nutrition experts, I wish to praise the key role you must play in contributing to the well-being of children with clefts. Lack of awareness about clefts means that, in some instances, recommended infant and young child feeding (IYCF) practices are overlooked and these children do not receive optimal feeding and nutrition care. As nutrition specialists, you should feel empowered to take the lead to ensure that mothers have the help they need to overcome feeding difficulties and that recommended IYCF practices are upheld.






